A LensDirect guide to keeping your eyes healthy (and complication‑free!)
Key Takeaways:
- Sleeping in contact lenses — whether a full night or a “quick nap” — raises the risk of a contact‑lens–related eye infection by roughly 6–8×. About one‑third of wearers report sleeping or napping in their lenses. Please don’t be one of them. (CDC)
- Even lenses labeled “extended or overnight wear” carry higher risk than removing lenses nightly, and they should be used only under professional guidance. (U.S. Food and Drug Administration)
- Smart habits that lower risk: remove lenses before sleep, keep lenses away from all water, rub/rinse with fresh disinfecting solution, and replace your lens case every 3 months. Consider daily disposables for maximum convenience — still not for sleeping. (CDC)
Why sleeping in contacts is risky (the short science)
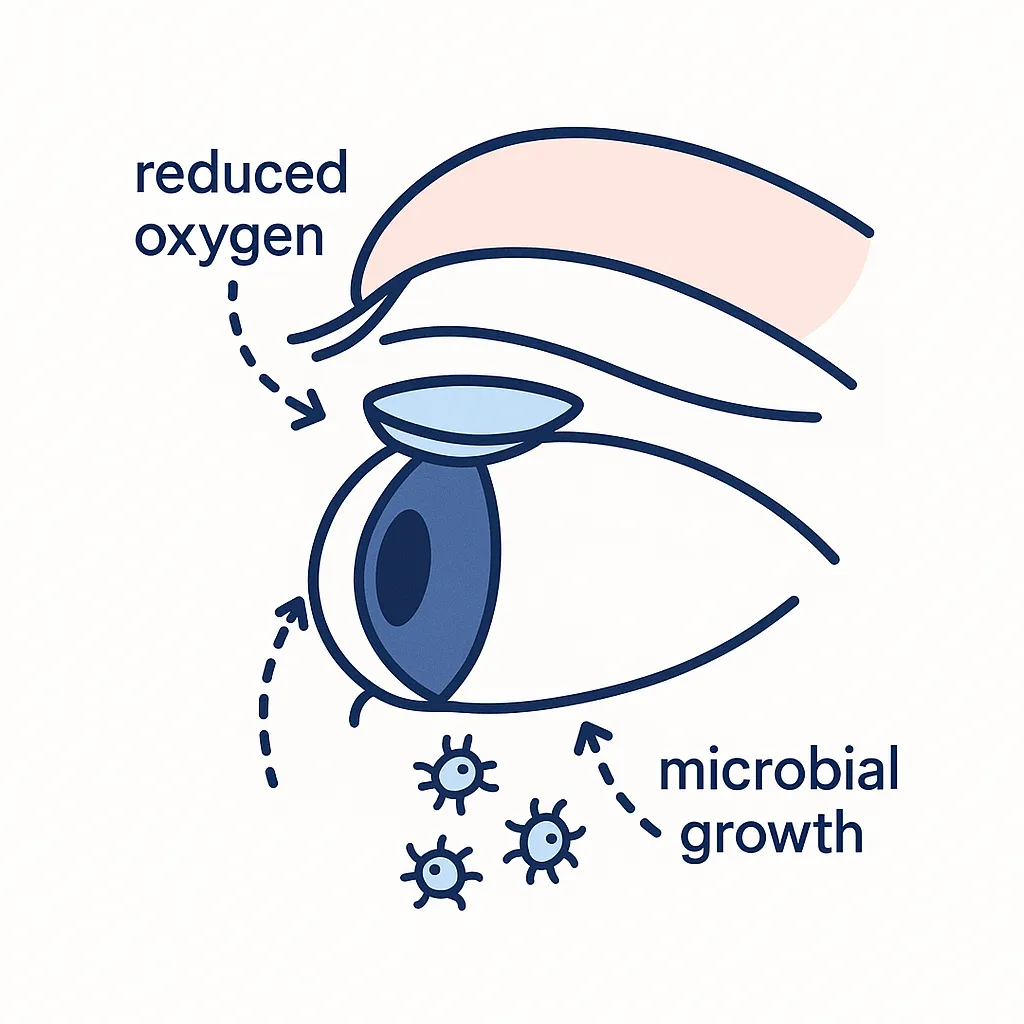
When you close your eyes, your cornea (the clear front window of your eye) receives less oxygen.
A contact lens — especially under a closed eyelid — reduces oxygen even further and limits natural tear exchange that flushes away microbes and debris.
That low‑oxygen, low‑flow micro‑environment stresses the corneal surface and makes it easier for bacteria, fungi, and amoebae to gain a foothold.
Translation: more irritation, inflammatory events, and a significantly higher chance of infection. Public‑health data consistently identify overnight lens wear as one of the riskiest behaviors for lens users. (PMC)
How risky are we talking?
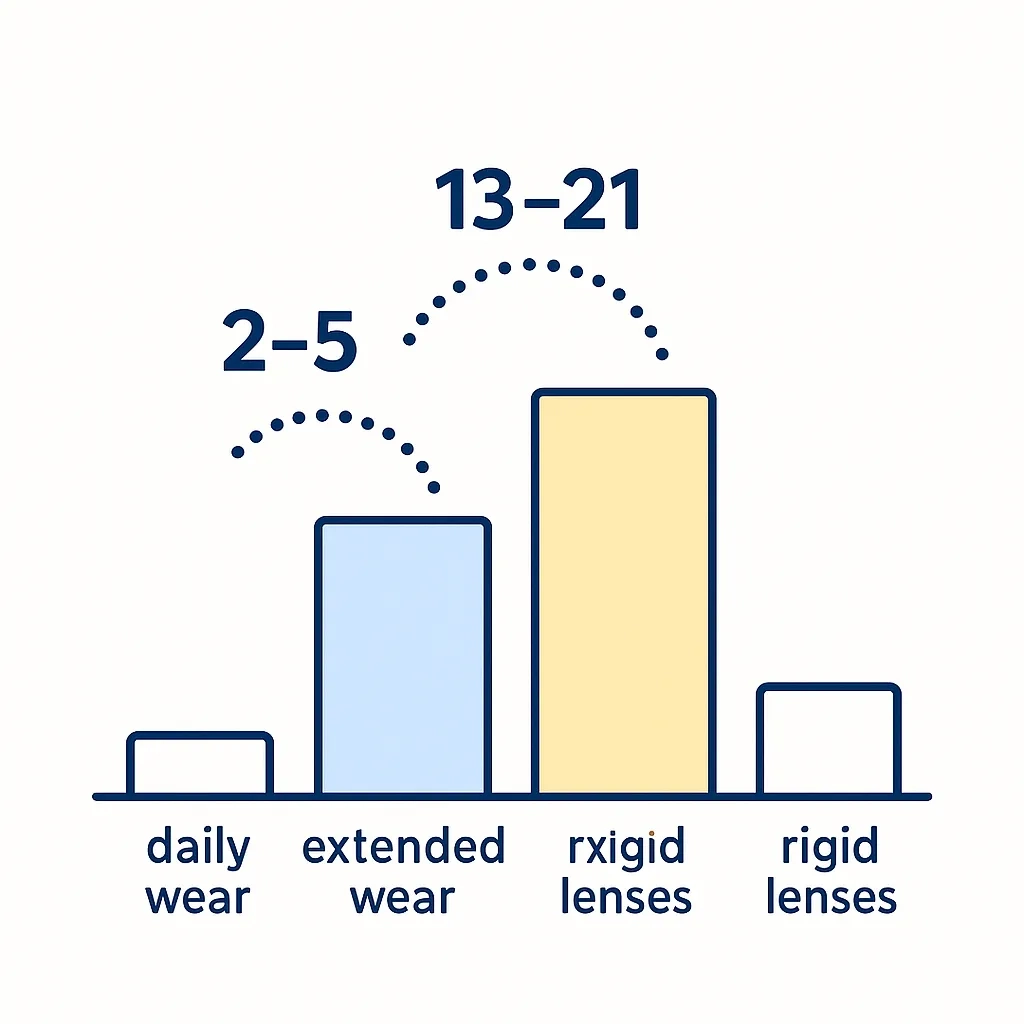
Large epidemiology studies estimate that, among soft lens wearers, daily wear has a microbial keratitis incidence of roughly 2–5 per 10,000 wearers per year, while extended/overnight wear jumps to ~13–21 per 10,000. Rigid gas‑permeable lenses generally show lower risk than soft lenses in daily wear, but any overnight use increases risk. (PubMed)
Modern silicone‑hydrogel materials deliver more oxygen, but they do not eliminate the overnight risk.
A U.S. post‑market study of silicone hydrogel lenses approved for up to 30 nights of continuous wear reported ~18 per 10,000 presumed microbial keratitis annually and rates comparable to older extended‑wear hydrogels.
In other words: better oxygen ≠ zero risk. (PubMed)
The Centers for Disease Control and Prevention (CDC) sums it up clearly: sleeping in lenses — inadvertently, occasionally, or as part of an “approved” schedule — increases infection risk six‑ to eightfold. (CDC)
“But my lenses say ‘extended wear’ — is it ever okay?”
Some soft and a few rigid lenses are FDA‑approved for overnight wear ranging from 1–6 nights up to 30 days, but this approval reflects what the lenses can do under careful clinical supervision, not that they’re as safe as nightly removal. If your eye care professional prescribes extended wear for specific reasons (e.g., work shifts), follow that plan exactly, keep your follow‑ups, and stop wear at the first sign of trouble. (U.S. Food and Drug Administration)
Even the FDA cautions that lenses worn during sleep — soft or rigid — carry a substantially greater risk of severe eye infection and potential vision loss compared with daily wear. (U.S. Food and Drug Administration)
If you accidentally slept in your contacts
- Don’t peel off a dry lens. Instill sterile saline or rewetting drops, wait a few minutes, then remove gently. Never use water. (CDC)
- Give your eyes a break. Switch to glasses for the day. If you use daily disposables, discard that pair and don’t reinsert a new one until your eyes feel normal. (CDC)
- Watch for red‑flag symptoms over 24–48 hours: increasing pain, light sensitivity, worsening redness, discharge, or blurry vision. If any appear, stop lens wear and call your eye doctor immediately — corneal infections can threaten vision. (American Academy of Ophthalmology)
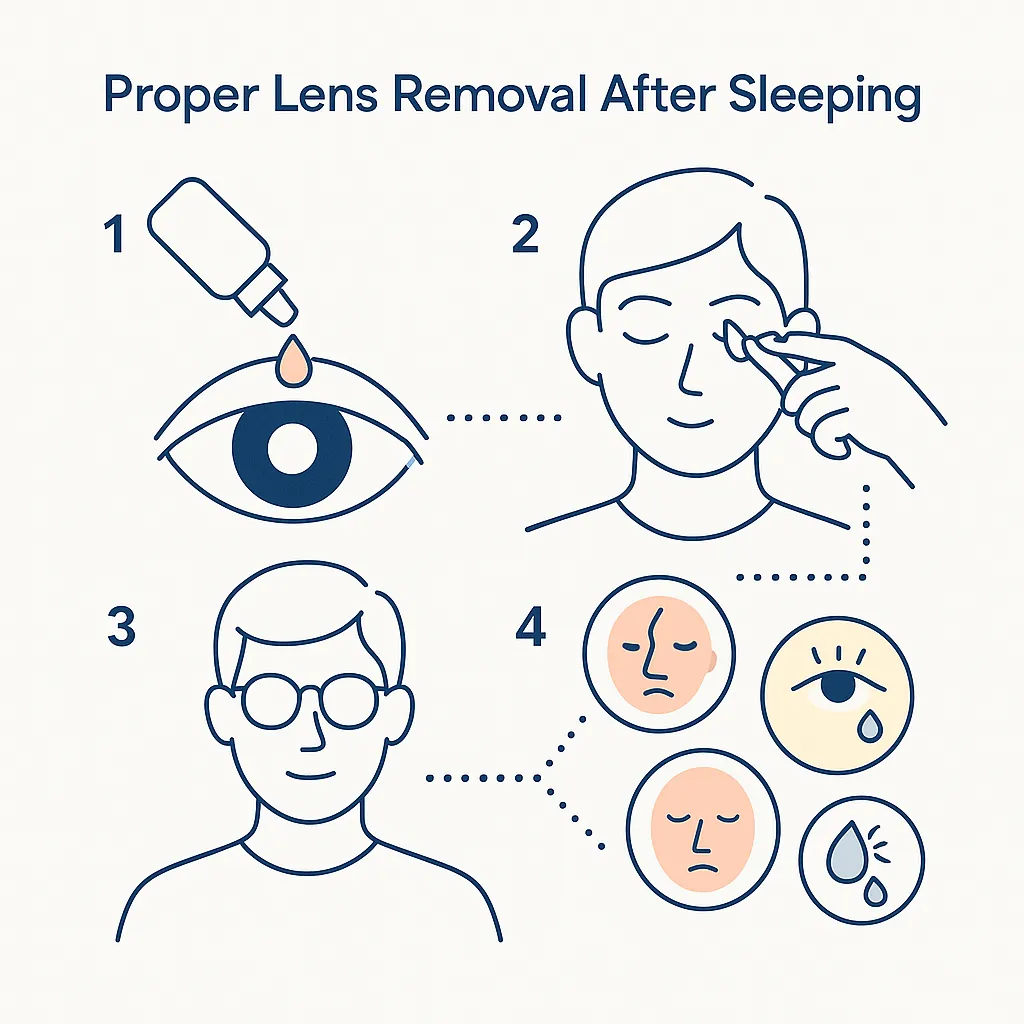
Safer, smarter alternatives (without sacrificing convenience)
1) Daily disposable lenses (single‑use)
For many people tempted to “doze and deal later,” daily disposables are a safer routine: fresh, clean lenses every morning, no case or solution to maintain.
They’re still not for sleeping, but they reduce hygiene pitfalls and have been associated with lower risk of Acanthamoeba keratitis compared with reusable lenses when worn as directed. (PubMed)
2) Nightly removal + meticulous hygiene
If you wear reusables (bi‑weekly or monthly), build a friction‑based cleaning habit: rub and rinse each lens with the recommended disinfecting solution; never top‑off old solution; and air‑dry your case upside‑down with caps off.
Replace your case every 3 months — biofilms love old cases. (CDC)
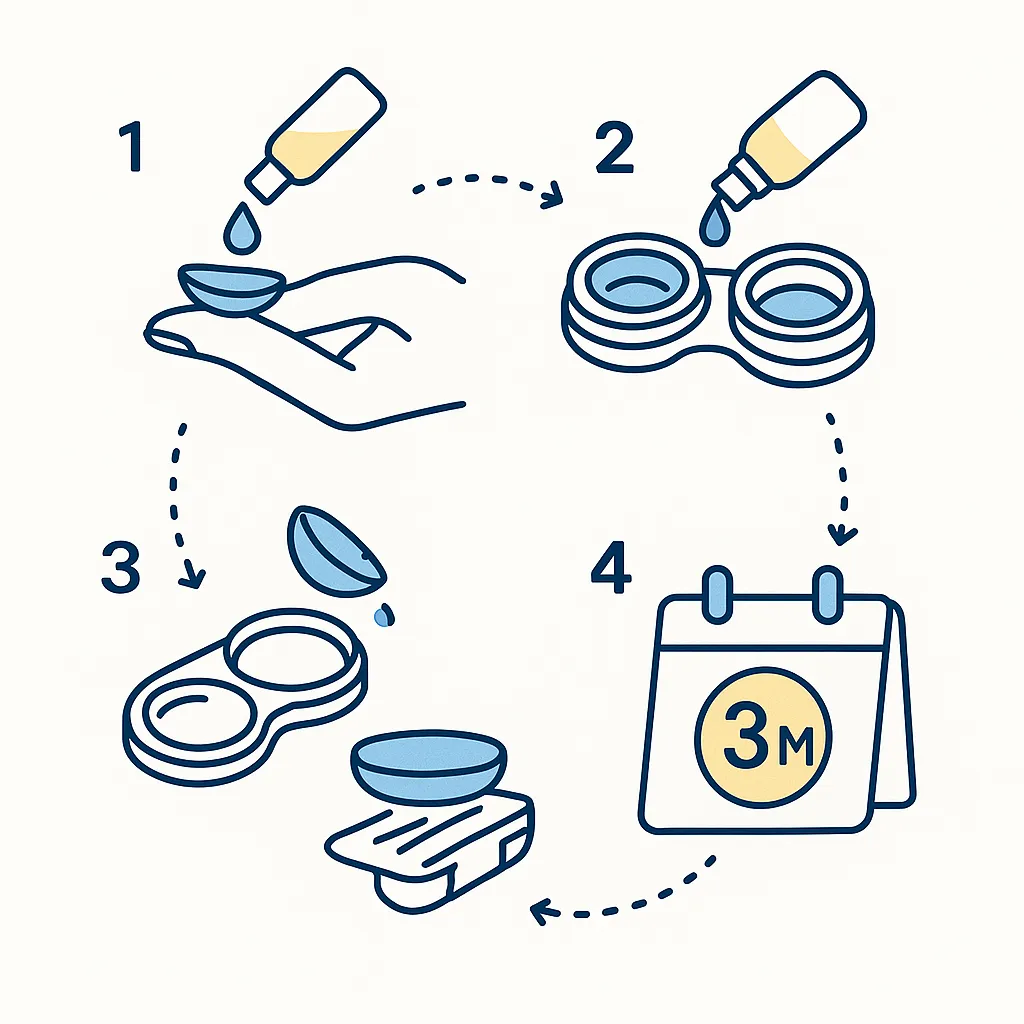
3) Keep lenses away from all water
Tap, pool, lake, ocean, or hot tub — water harbors organisms (notably Acanthamoeba) that cling to lenses and can cause devastating infections.
Remove lenses before water exposure; if water contacts a lens, take it out and either discard (dailies) or clean/disinfect overnight before reuse. (CDC)
4) Consider the right material — but not as a “sleep pass”
Silicone‑hydrogel lenses provide higher oxygen for daytime comfort, but overnight risk remains elevated.
Keep the benefit (comfort) and skip the risk (sleep). (Nature)

A quick reference: what to do (and what to avoid)

Do this:
- Remove lenses before sleep — every time.
- Wash and dry hands before handling lenses.
- Rub and rinse reusables; fill case with fresh disinfecting solution each time.
- Air‑dry the case (caps off) and replace every 3 months.
- Carry backup glasses for unplanned removals. (CDC)
Avoid this:

Extra‑credit good deeds: the environmental angle
Don’t toss used lenses down the sink or toilet. Research suggests 15–20% of wearers have flushed lenses, contributing to microplastics after wastewater processing. Instead, place used lenses in the trash (or use approved recycling programs when available). (ASU News)
The LensDirect take
We love contact lenses because our customers love what they enable — sports, travel, and everyday life without frames. The numbers don’t lie: approximately 45 million people in the U.S. wear contact lenses — plenty of reasons to spread good habits But safe wear isn’t optional; it’s part of the prescription. To stack the odds in your favor:
- Remove lenses every night.
- Keep water off your lenses — always.
- Choose the wear schedule that fits your habits. If convenience is king, talk to your provider about daily disposables (and remember: not for sleeping).
- Stock the basics: a fresh case (every 3 months), the right disinfecting solution, and a pair of current glasses in your bag or nightstand. (CDC)
- Bottom line: Sleeping in contacts changes the eye’s environment in ways that make infection more likely — by a lot. Nightly removal plus smart hygiene is the simplest, safest routine. If you need an overnight solution, that’s a medical decision — make it with your eye care professional and go in with clear eyes about the trade‑offs. (CDC)


Frequently Asked Questions
Is a short nap okay?
No. The risk increase applies to any sleeping in lenses, even naps. If you nod off with lenses in, remove them properly when you wake and give your eyes a break. (CDC)
Do daily disposables make sleeping in lenses safe?
No. Dailies simplify hygiene but must be removed before sleeping. Sleeping in any lens type increases infection risk. (U.S. Food and Drug Administration)
Are silicone‑hydrogel lenses safe to sleep in?
They deliver more oxygen, but research shows overnight silicone‑hydrogel wear has similar infection rates to older extended‑wear hydrogels. Better oxygen doesn’t erase overnight risk. (PubMed)
What about scleral lenses or specialty lenses?
Scleral and other specialty lenses are fantastic for certain eye conditions, but overnight wear is generally not recommended outside specific therapeutic indications — and still carries increased infection risk like any contact lens used during sleep. Follow your specialist’s instructions closely. (eyewiki.org)
Is orthokeratology (Ortho‑K) a safer way to sleep in lenses?
Ortho‑K uses rigid lenses overnight to temporarily reshape the cornea so you can see clearly by day without lenses. It can be effective when properly prescribed and monitored, but overnight lens wear remains a risk factor for infection; safety depends heavily on scrupulous hygiene and follow‑up. (In the U.S., Ortho‑K is approved for overnight wear; it is not specifically approved for myopia control.) Discuss with your provider whether Ortho‑K fits your needs and risk tolerance. (Lippincott Journals)
What symptoms mean “see a doctor now”?
Redness that’s getting worse, eye pain, light sensitivity, discharge, or sudden blur — especially after sleeping in lenses — warrant prompt evaluation. Don’t mask symptoms with “redness‑relief” drops; stop lens wear and contact your eye doctor. (American Academy of Ophthalmology)
Does smoking or poor hygiene matter?
Yes. Studies link smoking and noncompliant behaviors (like poor hand hygiene) with higher rates of contact‑lens complications. But the single riskiest behavior remains overnight wear. (PLOS)
How many people wear contacts, anyway?
Approximately 45 million people in the U.S. wear contact lenses — plenty of reasons to spread good habits. (CDC)
Sources & further reading
- CDC: About Contact Lenses; Risk behaviors & prevention; Water and lenses don’t mix; Case replacement every 3 months. (CDC)
- FDA: Types of Contact Lenses (extended wear); Consumer update on overnight risk. (U.S. Food and Drug Administration)
- Peer‑reviewed: Incidence by modality and extended‑wear silicone hydrogel risk (Ophthalmology 2005; reviews by Liesegang, Stapleton). (PubMed)
- Acanthamoeba risk & daily disposables: Carnt et al., Ophthalmology 2023; AAO EyeNet summary. (PubMed)
- AAO patient pages on corneal ulcers and contact lens infections (when to seek care). (American Academy of Ophthalmology)
This article is for informational purposes and does not replace professional medical advice. If you have symptoms or concerns, contact your eye care professional promptly.
Subscribe to our email newsletter to get the latest posts delivered right to your email.

